Long-Term MADRS Tracking: Your Personalized Monitoring Guide
March 10, 2026 | By Elias Monroe
Understanding depression is not about looking at a single moment in time. For most people, mental health is a journey with many peaks and valleys. Because symptoms fluctuate, a one-time assessment often fails to capture the full picture. You might wonder: how can you tell if your treatment is actually working over several months? This is where long-term tracking becomes essential.
The Montgomery-Åsberg Depression Rating Scale (MADRS) is a world-class tool used by clinicians to measure the severity of depressive symptoms. By using this scale regularly, you can move away from guessing how you feel and start looking at real data. Whether you are a healthcare professional or someone managing your own mental health, having a clear record of your progress is vital. You can start your test today to begin building this valuable history of your emotional well-being.
Let's explore how to create a monitoring schedule tailored to your specific needs. We will examine how to interpret your scores over time and use that data to drive better decisions with your healthcare provider. We designed this guide to help you leverage the MADRS framework for meaningful insights into your recovery.
![]()
Creating Your MADRS Monitoring Schedule
Consistency is the most important part of long-term tracking. If you only take a test when you feel very low, your data will be biased. To get an accurate view of your health, you need a plan. A well-structured schedule helps you identify patterns that you might otherwise miss. It allows you to see if your "good days" are becoming more frequent or if your "bad days" are tied to specific events.
Determining Optimal Assessment Intervals for Different Clinical Scenarios
The frequency of your assessments depends on your current situation. If you have just started a new medication or therapy, you are in an "acute phase." During this time, experts often recommend taking the MADRS online test once a week. This weekly testing helps you and your doctor track how quickly you're responding to treatment. It also reveals whether side effects might be affecting your mood.
For those who have been on a stable treatment plan for several months, the "maintenance phase" begins. In this stage, checking in once every two to four weeks is usually enough. This frequency is high enough to catch a potential relapse early. It is also low enough that it does not feel like a daily burden. If you are a researcher, your intervals might be even more specific, following exact study protocols.
Tools for Setting Reminders and Tracking Consistent Assessments
It is easy to forget to check in when you are busy or feeling better. This is why using digital tools is so helpful. Many people use smartphone calendars or specialized health apps to set recurring alerts. Consistency ensures that your longitudinal data remains reliable. Without a steady stream of data, it is hard to distinguish between a temporary mood swing and a clinical trend.
The MADRS.net platform is designed to make this process easy. Regular use of our depression scale lets you quickly answer 10 core questions for an instant score. Having a dedicated digital platform for your assessments eliminates monitoring friction. Easy access increases your likelihood of maintaining this important monitoring habit over time.
Seasonal Considerations and Life Events in Depression Monitoring
External factors often play a huge role in how we feel. Many individuals experience Seasonal Affective Disorder (SAD), where symptoms worsen during the winter months. If you know you struggle with seasonal changes, you might increase your monitoring frequency during autumn. This proactive approach allows you to adjust your treatment plan before the symptoms become overwhelming.
Life events like job changes, moving house, or losing a loved one also require closer monitoring. These stressors can trigger a dip in your mental health. By tracking your scores during these times, you can see exactly how much your internal state is being affected by external pressure. This data is incredibly useful for your therapist. It provides a factual basis for your discussions rather than relying on memory alone.
Interpreting MADRS Score Trends Over Time
Once you have collected data over several weeks or months, the next step is interpretation. A single score tells you how you feel today. A trend line tells you where you are headed. Understanding these trends is the key to knowing if you are on the right path or if your treatment plan needs a revision.
What Constitutes Clinically Significant Change in MADRS Scores
Not every small change in your score is cause for alarm or celebration. The scale ranges from 0 to 60. Generally, a score between 0 and 6 is considered "normal" or in remission. A score of 35 or higher indicates "severe depression." But what does a change of 5 points mean? In clinical settings, a "response" to treatment is often defined as a 50% reduction in your initial score.
A "clinically significant" change is one that actually impacts your daily life. For example, if your score drops from 30 to 22, you might notice you have more energy for work or social activities. When you see your results on our site, look for these steady shifts. If your score stays the same for a long time despite treatment, it may be a sign that the current approach is not as effective as it could be.
Visualizing MADRS Data: Charts, Graphs, and Pattern Recognition
Humans are visual creatures. It is much easier to understand a line graph than a list of numbers. When you plot your scores on a graph, patterns emerge. You might see a "sawtooth" pattern, where your mood jumps up and down frequently. Or, you might see a "downward slope," which is the goal of most treatments.
Visualizing your data helps you identify triggers. For instance, you might notice that your score always rises at the end of every month. This could be related to work deadlines or financial stress. Recognizing these patterns allows you to plan self-care activities in advance. You can check your progress using our digital tools to keep these visualizations accurate and up to date.
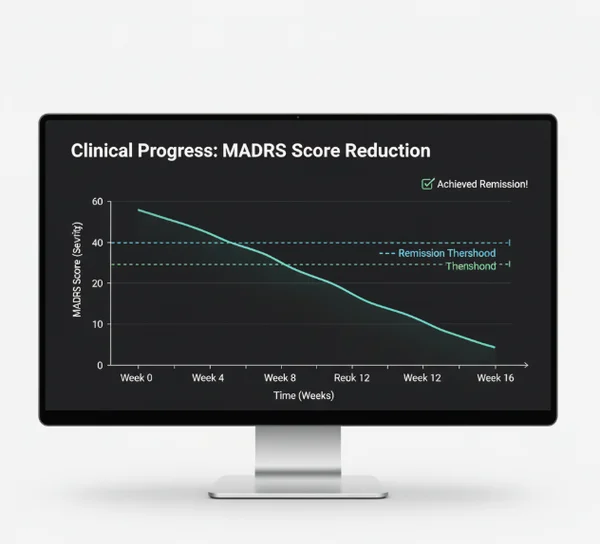
Distinguishing Between Response and Remission Using Longitudinal MADRS Data
There is a big difference between feeling "better" and feeling "well." In the world of mental health, "response" means your symptoms have decreased significantly. However, you might still have some lingering sadness or sleep issues. "Remission," on the other hand, means your symptoms have almost entirely disappeared. This usually results in a score of 6 or lower.
Long-term tracking is the only way to confirm remission. A single low score could just be a very good day. True remission occurs when your scores stay consistently low for several months. Tracking this data gives you the confidence to say that your recovery is stable. It also provides a "baseline." If symptoms ever return, you can catch them immediately by noticing a rise from your stable baseline.
Personalized Assessment Planning for Optimal Outcomes
No two people experience depression the same way. Therefore, your monitoring plan should be as unique as you are. By personalizing how you use the scale, you ensure that the data you collect is actually useful for your specific goals.
Customizing MADRS Monitoring for Specific Treatment Modalities
Different treatments work at different speeds. If you are taking fast-acting treatments, daily or every-other-day tracking might be necessary for a short time. If you are in long-term talk therapy, your progress might be more gradual. In this case, monthly tracking allows you to see the "big picture" of your emotional growth over the years.
Some treatments specifically target certain symptoms, like sleep or concentration. Since the scale covers 10 specific areas, you can look at the sub-scores for each question. If your total score is going down but your "sleep" score remains high, you can discuss this specific issue with your doctor. You can take the test to see which specific areas of your life are most affected right now.
Incorporating MADRS Data into Shared Decision-Making Processes
Shared decision-making occurs when you and your doctor work as a team. Instead of the doctor just giving instructions, you bring your tracking data to the table. When you can say, "Look at my scores from the last three months; my sadness is better, but my appetite is still very low," you provide high-quality evidence.
This approach reduces the risk of miscommunication. Sometimes, when we are at the doctor's office, we forget how we felt two weeks ago. Having a recorded history of your scores ensures that the doctor sees the truth, not just how you feel in that specific 15-minute appointment. This leads to more accurate medication adjustments and better therapy outcomes.
Digital Tools for Enhanced MADRS Monitoring and Analysis
Modern technology has transformed how we monitor mental health. You no longer need to carry a paper chart or try to remember your scores. Digital platforms offer privacy, speed, and accuracy. At MADRS.net, we provide an online assessment that follows the clinical gold standard. Our tool is designed for mental health professionals and individuals who want a reliable way to measure their symptoms.
One of the greatest advantages of digital tools is the ability to generate a comprehensive report. While the standard score is helpful, a detailed analysis looks at your answers in the context of your background. This provides a deeper level of insight into your challenges and strengths. By using these advanced tools, you turn a simple test into a robust mental health strategy.
Achieving Stability Through Data
Long-term MADRS tracking is one of the most powerful things you can do for your mental health. It transforms a subjective feeling into objective data. By creating a consistent schedule, learning how to interpret your score trends, and personalizing your plan, you gain control over your recovery journey. You no longer have to wonder if you are getting better; you can see it in your results.
While depression itself is complex, tracking your progress can be straightforward with the right tools. Use the resources available to you to stay informed and proactive. Whether you are a clinician looking to help your patients or an individual seeking clarity, this scale is a trusted companion. Start tracking your symptoms today and take the first step toward a more data-driven and effective approach to mental wellness.
The Takeaway
How often should I complete a MADRS assessment for effective monitoring?
For most people, completing an assessment once every week or every two weeks is the best balance. If you are going through a major treatment change, your doctor might suggest more frequent checks. Once you feel stable and are in the maintenance phase, once a month is usually sufficient. You can use our tool whenever you need to check your current status.
What does a decrease of 5 points on my MADRS score actually mean?
A 5-point drop is generally considered a positive sign, but its meaning depends on your starting point. If your score was 40 and it is now 35, you are still in the "severe" range, but you are moving in the right direction. If your score was 12 and it is now 7, you are very close to full remission. Always look at the percentage of change and how it matches your daily feelings.
Can I monitor my depression with MADRS if I'm not currently in treatment?
Yes, absolutely. Many people use the scale for self-monitoring to understand their own emotional patterns. It can help you decide when it might be time to seek professional help. If you notice your scores are consistently rising or staying in the moderate-to-severe range, it is a clear signal to reach out to a healthcare provider.
How can I best discuss my MADRS tracking data with my mental health provider?
The best way is to bring a printed or digital copy of your score history to your appointment. Point out specific dates where your score changed significantly and explain what was happening in your life at that time. This helps your provider see the "why" behind the numbers. Using a standardized test makes it much easier for your doctor to understand your progress quickly.